Let’s be honest, counterfeits are like weeds. No matter what you do, they tend to pop back up. As a reported $75 billion dollar enterprise that costs the U.S. between $200-250 billion a year, it’s no wonder counterfeiting is still an active “enterprise.”
Many counterfeiters saw a great opportunity for growth during the 2020-2022 semiconductor shortage. Industry leaders predict the shortage to continue at least partway into 2023. This means that suspect counterfeits are a bigger risk now than ever before. That goes for every sector of business that relies on electronic components. No matter how tough the regulations are or how big a company is, counterfeiters aren’t choosy. Suspect components can enter a supply chain at any time, they just need an opening. The pandemic gave them dozens.
In early Feb. 2022 counterfeit components were found in the supply chain for several nuclear power plants. In the spring of 2021, BotFactory Inc. a 3-D printer manufacturer bought components off AliExpress, all counterfeit and unusable. An investigation carried out by the Senate Armed Services Committee in 2012 found more than one million counterfeit electronic components had been used in equipment designed for the U.S. Air Force, Navy, and Special Operations.
These few instances of counterfeit components made the news. The true extent of counterfeit component damage, beyond cost, is unimaginable. If counterfeit components can slip into equipment designed for military use, healthcare is just as vulnerable.
Worse, counterfeit components in medical devices are a matter of life and death.
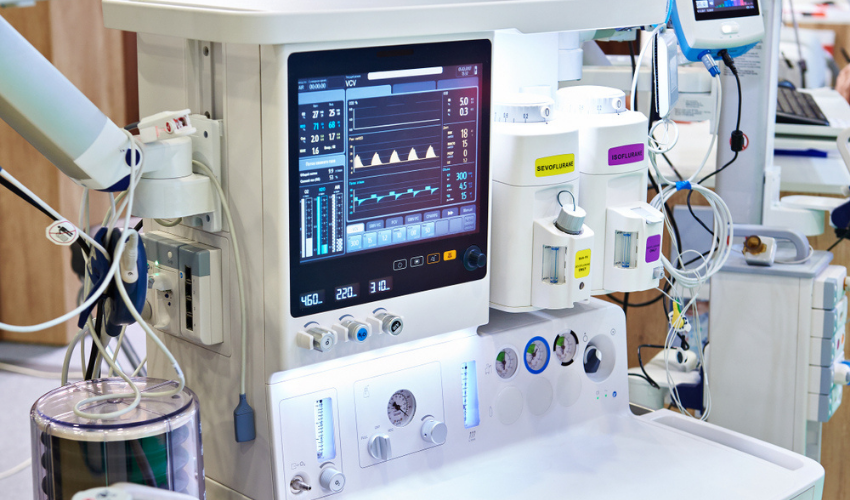
Medical Devices: The Technology That Saves Lives
Medical devices in healthcare cover a vast range of appliances, all performing different functions at different sizes for a single purpose: patient health. Biomedical devices are classified into individual categories that are decided by patient risk. What this means is that if a device were to cease operation or become partially inoperable, how large of a risk does that pose to a patient’s life?
As an example, Class I devices pose a low or moderate risk to patient health. Class I medical devices represent 47% of all would include many non-electronic devices such as tongue depressors, bedpans, and elastic bandages. If any of these were to malfunction in some way, the risk to patient life is minimal. Class II medical devices are rated as having a moderate to high risk. These devices include powered wheelchairs, blood pressure cuffs, and blood transfusion kits.
It’s important to note that many Class I and Class II medical devices are mostly not electronic in nature. Class III medical devices are rated as having a high risk to patient life if malfunction or interoperability was to occur. These devices usually support life and represent 10% of medical devices regulated by the FDA. The list of Class III medical devices includes pacemakers, high-frequency ventilators, implanted prosthetics, and cochlear implants.
In order to go to market, these Class III products must go through the rigorous FDA Premarket Approval (PMA) process to prove safety and effectiveness. This includes clinical trials, data collection, and a substantive review of quality systems over a long time period. It is said to be one of the most intensive approval processes out there. If anything was to change after approval, such as an electronic component going into obsolescence and a substitute being needed, this process must be repeated.
One can imagine the importance of managing obsolescence in such a strict industry. Where one small component change means over 45 days of testing to recertify a device. When faced with a sudden lack of a component and no time to go through the PMA process again, what happens?
Counterfeiters see an opportunity.
How Do Counterfeits Enter a Strictly Regulated Industry?
If strict regulations were the only thing necessary to keep counterfeiters out, that gray market wouldn’t be as large as it is today. Counterfeit components slipping into military products, as discovered by the Senate Armed Services Committee in 2012, wouldn’t be an issue.
In 2012, the world wasn’t in a global pandemic. There was no semiconductor shortage, and the semiconductor market was experiencing normal growth and some decline in sales. Yet, counterfeit components totaling one million still entered the supply chain and found their way into military product manufacturers’ hands.
Now, imagine how bad the counterfeit damage will be looking back on the 2020-2022 semiconductor shortage. Global shortages work to a counterfeiter’s benefit. Stalled production costs from the pandemic and shortage are expected to reach over $500 billion. That kind of damage can make or break a company. Many businesses did in fact close permanently in response.
The healthcare industry, which usually makes up only 11% of industrial semiconductor orders a year, and only 1.3% of semiconductor sales around the world, faced a sudden uptick in electronic component demand. As it happens, the main catalyst being the semiconductor shortage and the Covid-19 pandemic put many people in the hospital. Covid-19 has a tremendous impact on a patient’s ability to breathe the demand for ventilators skyrocketed.
Most ventilators need electronic components to function properly. Ventilators, under the FDA’s medical device rating system, are rated as Class III devices. The need for Class III medical devices rose during the pandemic. Component obsolescence and global component shortages are hard enough obstacles on their own. Together, they become a monumental problem – one that many healthcare product manufacturers have faced over the past two years.
The pandemic presented a golden opportunity to counterfeiters. No matter how strictly an industry regulates itself, those within it must always be prepared to encounter and mitigate the risks.
Ways to Combat the Counterfeit Risk
The counterfeit risk is dangerous and persistent, but not unbeatable. Diligence is a requirement and constant improvement in assessing and testing the more sophisticated counterfeits to ensure they don’t enter your supply chain is necessary. Medical device manufacturers have a leg up on consumer electronics because of the stringent requirements within the sector.
As we know, it is not a guarantee, but it makes it more difficult for suspect components to slip in, nonetheless. There are many tests that can be done to determine component authenticity, even by the medical product manufacturer. Certain tests, such as x-ray inspection or microscopic analysis, can verify authenticity.
It is better to buy from a distributor that has these kinds of tests available. X-ray inspections and scrape testing can help weed out even some of the most sophisticated suspect components. Distributors that are certified in SAE AS6081 have quality assurance systems in place that follow standardized requirements on how to detect, mitigate, and remove such components from supply chains.
Even with new ways to combat counterfeits, like barcodes, mass serialization, and anti-counterfeit package technologies that improve product tracking, it takes time to avoid risk on your own. That is why, in the face of counterfeit risks, buying from a distributor that is trained, certified, and up to date on the latest counterfeit methods is the best choice.
Your Best Option: An AS6081 Distributor
As an AS6081 electronic components distributor, Area51 Electronics has the testing equipment needed and the guidelines in place to ensure quality products. The semiconductor industry loses $7.5 billion to counterfeit components a year, and that number is set to increase from the global shortage.
Monetary losses from counterfeit component purchases aren’t the only problems with buying suspect components. Thousands of Americans lose their jobs due to counterfeiting. Taxpayers shelled out $2.7 million in 2010 when counterfeit components were discovered in mission computers for Terminal High Altitude Area Defense (THAAD) missiles.
Area51 Electronics not only knows how to avoid, detect, and mitigate risk by having AS6081 certification but also is part of the DLA Land and Maritime QSLD Program. This program is overseen by the Department of Defense (DoD) and held to strict standards and requirements. A distributor that takes every step possible to ensure the counterfeit risk is met, is what the healthcare industry needs.
So, you can focus on what’s important, saving lives.